Jeff Johnson

So you want to do COVID screenings at your office?
You need these lessons from the front lines
Just 12 short weeks ago only a few were paying attention to a virus on the other side of the world. PPE, social distancing, and flattening the curve weren’t thoughts, let alone words used in everyday conversation, and hand sanitizer and toilet paper were easy to come by. Business and the economy were booming. And as I write this, literally everything has changed. Businesses suspended operations as everyone’s focus has appropriately turned to flattening that curve, and now they’re starting to reopen. There is a deluge of information, but we still don’t really understand the invisible enemy we are fighting, and there is rampant disagreement regarding what to do about it.
However, there is one thing we can all agree on, and that is things will be different after this.
Similar to the way 9-11 changed the world forever, COVID-19 will change business as we know it. What we don’t know for sure, though, is what those changes will look like, and if they’ll be temporary or permanent.
Will we wear masks forever and never shake hands again? Probably not. However, one new addition to many businesses that might stick around for quite some time is temperature screenings at their entrances. Today, we’re seeing screening protocol at the doors of essential businesses. But as the economy’s doors reopen, we’ll seeing more screening checkpoints. And they’re really not being done correctly.
Change is hard, and unfortunately there are lots of problems with the makeshift screening systems getting rushed into place. Here’s what we’ve learned:
- When done correctly, checkpoint screenings cause little to no inconvenience (unlike other security bottlenecks you’re familiar with).
- Though it’s not perfect, measuring temperature is an easy way to catch at least some of
the symptomatic population before they cough and sneeze their way through your next
meeting.
- Screening devices will become increasingly affordable after the war for inventory ends.
If we look at Asian countries that are well-versed in dealing with outbreaks, we can see that temperature readings are everywhere. Many airports, factories, retail locations and even golf driving ranges have some form of temperature monitoring available. If these processes are going to take root in our way of life as well, we want to help. But who are we to play a part?
Before I associated the word “Corona” with anything other than a delightful beach beer, I was running a company that focused on helping employers lower their musculoskeletal claims costs by staffing healthcare providers onsite. We were growing quickly with some amazing clients, and our team of healthcare providers around the country were incredible at finding solutions to all forms of physical medicine challenges for our clients’ businesses. Then, almost overnight, we had to cease operations state by state. As we shuttered our operations, a client asked if we could use our provider onsite to do COVID-19 Screenings. I thought “how hard could that be?” They were already using HR to do the temp checks and ask questions, but the client wanted medically knowledgeable and skilled reinforcements. We learned quickly that there is way more to it than meets the eye. Below are some of the biggest considerations you should weigh as you build your own screening program.
- Who should do the screenings?
Assigning someone to the job sounds simple, right? Wrong! And, in fact, this might be the most critical consideration of all. With the economy on the ropes and many businesses missing their numbers, it’s tempting to get volunteers or throw this in HR’s lap. Maybe you’re thinking someone in accounting was a lifeguard back in the day, so they should do step into the screening post. Wherever your line of thought is going, I encourage you to think outside the office. With HIPPA, OSHA, CDC, WHO and everyone else who is trying to drive this ship releasing new guidelines daily, it’s tough for trained professionals to keep up, much less people who have other roles and responsibilities. We have seen the team member who was “voluntold” to help end up in literal tears from the increased hours and responsibilities, as well as the risk of exposure. That’s a big burden for an untrained individual, plus, it’s far from ideal for the business and can easily be avoided. At a minimum, if you are doing screenings internally, have your attorneys draft a document that the volunteers sign to hold the business harmless. But really there is no need to go that route; instead, consider a third party that is built to deal with those stressors and can problem-solve in real time when situations arise, because trust me, they will arise. When you have the right person in the role, they can think critically, as well as beyond the binary. For instance, if an employee shows up with an elevated temp, but a trained screener learns the employee’s truck doesn’t have working air conditioning, we can let the employee cool off, temp them again, and allow a healthy person get to work.
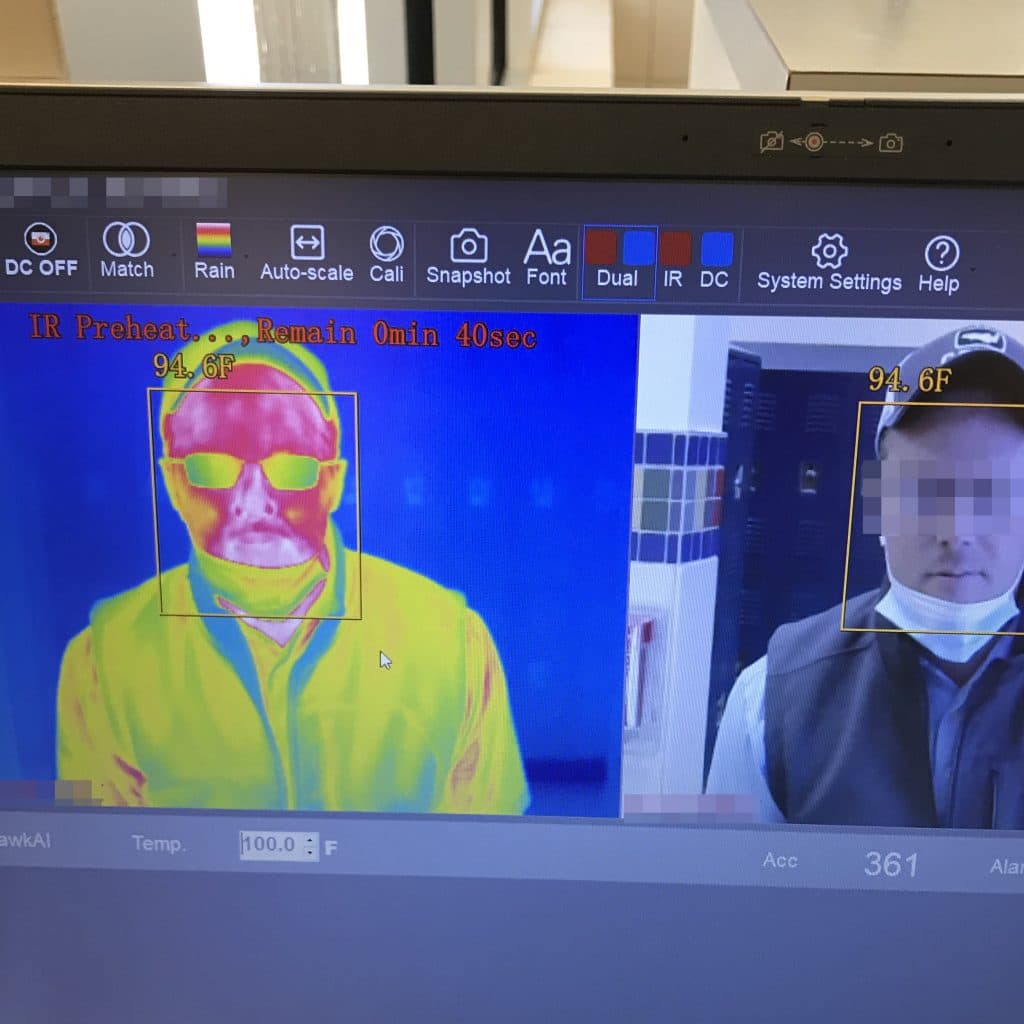
- Equipment matters!
Let’s start with the most egregious example we’ve seen to date. A well-intentioned company launched their screening process several weeks before we were contacted to evaluate them. A quick look at their thermometer and it was obvious that it wasn’t a great unit. After pressing the button a few times, we realized something was wrong; it was reading normal when we scanned a person or a water bottle and interestingly it just kept giving the same three temperatures no matter what surface you put it on. Not surprisingly, the company hadn’t identified a single fever in their employees with this knockoff. Yikes. It’s important that you have a dependable thermometer and that it has been calibrated or at least tested on a known temperature. Remember also that the ambient temperature can affect the reading and accuracy of your device. For instance, if you’re taking temps in the parking lot versus inside, you might need to adjust your device. We’ve found several devices that are over three degrees off on the calibration. This is often seen when someone is using a device that’s intended for mechanical purposes not human screening. So, invest in good devices, or invest in vendors that use good devices!
- Training is crucial
Though it might be obvious, some level of training is needed for whoever you decide to put in the screener position. That training should be, at the very minimum, on:
- how to wear PPE correctly
- how to perform a scan with the instruments provided
- how to check and calibrate the instrument
- how to manage the flow of traffic
- what to do if you have a high-risk employee
- what the steps are for sending someone home
- what to do if the employee refuses the screen
- what questions to ask, and so on
I could keep going, but you see that there is more involved than giving an employee the thermometer and sending them out front to defend the office.
- Design a solid process
When designing your screening process, it’s critical to ask these three questions: Is it effective? Is it efficient? Could you do it forever?
- effectiveness refers to taking a temperature, not diagnosing a condition. Is the device reliable and does the person wielding it know what they are doing? If so, then it should be effective at identifying an elevated body temp.
- efficiency measures the requisite amount of people screened without a significant delay. If you have a large factory and 500 or 5000 people are all showing up within the same one-hour window, a single employee will not be able to scan them with an IR thermometer fast enough. You can stagger arrival times to help with flow, but the third question helps eliminate short-term thinking.
- can you do this forever? If the answer is yes,that’s the mark of a good system. When designed and implemented correctly, the system should be effortless to maintain. If you’re creating a process that’s clunky, cumbersome, and irritating, you will struggle with compliance and morale, and your business and team will suffer needlessly as a result. Of course, I’m hopeful that we don’t have to do this forever, but again, we have no idea what our new normal will look like and how long it will stick around. As we analyze a new client’s facility, we often include a phase 2 component that includes turning over operations to local personnel. In this event, we’ve had the opportunity to run the system for them for a set period, train them in real time and become a resource for any questions moving forward.
Having a phase 2 or a simple source, setup, train and turnover model helps address the elephant in the room: cost. Cost is consistently reported as the biggest concern with screening programs. We’ve seen employers pricing units as high a $50,000 for subpar equipment like red light cameras. Fortunately, we’ve able to help many of them find superior options for a fraction of the cost. As you think through what a good screening program might look like, start with a budget in mind. Understanding that spending a little on technology on the front end can equal substantial savings in money and time.
I could go on for days with stories we’ve encountered, like about employees taking NSAIDS before the morning screening to dodge a high temp, and people taking work PPE home, or, worse, taking PPE out of the trash can. The good news is that we’ve seen a variety of human behavior and built a solution for it so you don’t have to.
I hope this has given you a few things to consider as we get back to work and navigate what the new normal looks like for businesses. If you need any help with design, implementation, sourcing or problem solving for your location, we are here for you.
Stay safe out there,
Jeff Johnson, D.C.
President
Cumulus Solutions
Today’s business leaders face a rapidly changing health and safety landscape, making it harder than ever to protect employees and businesses. With Cumulus as your expert corporate health and wellness partner, we solve your healthcare challenges so your company and teams can thrive.